|
*Please note that even though this was published on January 28, 2017, I shared this at the Cabin on September 10, 2016.*
I didn’t give myself the opportunity to be scared. Superior mesenteric artery syndrome has a 1-in-3 mortality rate without proper treatment, and surgery is the only proper treatment. I just ignored that fact that I could die and went on with my life as well as I could manage. I was literally starving to death and I completely ignored it. That was how I handled my situation then, and now it hurts me to think that. While I was in the hospital, I handled things fairly well. When I was told that I would need to have another surgery because I had a complete obstruction, which happened twice, I would be able to pull through and convince myself that I could do it. At one point, the doctors were stumped and were giving us plans of permanent feeding via a tube inserted directly into my abdomen, and I was able to handle it, because in a way, I ignored it. When little things happened I would break down. My ng-tube leaked bile all over me, and I cried I was so upset. For one of my tests, which required me to drink barium, was scheduled after I had gone two weeks in the hospital without eating or drinking anything except a bowl of chicken broth that I threw up. Instead of being able to drink the barium, it was put down my ng-tube, and I cried. I cried because I wasn’t allowed to drink barium. In a sense, I have been traumatized by what has happened to me. I was away from home for three weeks straight, and I was able to endure so much. I’ve experienced more pain than I ever thought was possible. Both physical and emotional pain. When my bowel was dying because of a complete obstruction caused by an adhesion, I experienced abdominal pain so severe that not even a narcotic painkiller could take an edge off of it. After my first surgery I experienced extreme chest pain and intense abdominal pain that was even worse than when my bowel was dying. It was so bad that I could barely breathe, and my arms and legs locked up, went numb, and I could barely move my fingers and toes. During those times I clung to Exodus 14:14, “The Lord will fight for you, you need only be still.” And to the lyrics by Jeremy Camp that say, “There will be a day with no more tears, No more pain, and no more fears There will be a day when the burdens of this place Will be no more, we'll see Jesus face to face.” Even now, during my recovery I still cling to God’s promises. One of them specifically from Revelation 21:4-5 says, “He will wipe away every tear from their eyes. Death will no longer exist; grief, crying and pain will exist no longer, because the previous things have passed away. Then the One seated on the throne said, ‘Look! I am making everything new.’ He also said, ‘Write, because these words are faithful and true.’” Even though I am suffering now, there is a promise of eternity that excludes all pain and suffering. Hope is greater than fear, and I will always have the hope of Jesus’s coming. I was asked during and after my hospital stays, “Where do you find your joy?” There were points where I couldn’t use the bathroom with help or even sit up in bed without having to be helped. Where did my joy come from? I couldn’t find it with eating or being healthy. I discovered the hard way that my joy comes from the Lord and that no earthly pleasure, no matter how small, should stand in the way of the Lord. Psalm 16:11 says, “You make known to me the path of life; in your presence there is fullness of joy; at your right hand are pleasures forevermore.” I relied on the strength of the Lord more than I had ever before in my life, and I found the true meaning of joy. People sacrificed a lot for me during my hospitals stays. I did not think much of it at the time, but looking back I feel guilty. Not only did being sick affect my summer, it ruined others’. My grandparents lived with us for five weeks during my first hospital stay and came down again when I was hospitalized again for my third surgery. We were supposed to visit them that weekend. My mom literally lived at the hospital with me on weekdays and sometimes a few days went by before she even made it home. Dad stayed with me on the weekends, and during the weekdays he went straight to the hospital after work, stayed until after ten, went home to do hours more of charting, and was at the hospital by 6:30 the next morning to see the doctors round. Both parents pulled all-nighters or got less than 4 hours of sleep on nights in the ER or on nights when my health went downhill fast. My brother and sister had to be self-sufficient when our parents were gone with me. They had many meals alone and even had to spend a night at home alone when an emergency ER visit became everyone’s greatest concern. Friends visited too. Some did on top of working 40 hour weeks and others stayed late at night to pray when we weren’t sure if I was going to get better and when the doctors were stumped at my condition. During the three weeks of my first hospital stay, over 70 people visited, and many came more than once. I received dozens of cards and many gifts too. I could never express how thankful I was and still am for all of the visitors and support, but at the same time I still feel guilty. Why would everyone, especially my parents, do all this for me? I don’t deserve any of it. I asked one of my friends this question when I became overwhelmed with everything that had happened and his answer was, “Because they love you.” Everyone was showing love and compassion for me. Anther friend pointed out that if all these people love you so much that they would literally do anything for you, imagine the love that Christ has for all of us. John 15:13 states, “Greater love has no one than this, that he lay down his life for his friends.” 1 John 3:16 says, “This is how we know what love is: Jesus Christ laid down his life for us.” Jesus is our friend and he showed His love by laying down His life for us. I was shown so much love during this experience and it truly changed me. When I was in the hospital, my parents were willing to literally do anything for me or give me anything I wanted. Those acts of kindness made me feel awful because I had nothing to deserve that type of treatment, and because what I wanted more than anything couldn’t be given to me by anyway. I wanted to be well. I wanted to be home. I wanted all the tubes and IV’s to be gone. I wanted to take a real shower. I wanted to stop throwing up liters of bile. I wanted to eat, especially without pain, nausea, and vomiting. Now, I want to live without the fear of having to go the ER or even having to have another surgery, which I’m reminded of every time I throw up bile. Even now I am still not back to normal, or maybe I have already reached my new normal. I never feel hungry, and most of the time I force myself to eat because I know I need to. Food is still not very appealing, and I do have discomfort, and sometimes even nausea whenever I eat. Ever since my third surgery, about every two or three weeks, I get blocked up to the point that my abdomen will swell up so much that some of my clothes won’t fit me, and I’ll throw up, sometimes even bile. Then, I’ll have to go either to the doctor or the ER, get cleared out, and start all over again. As of right now we’re trying to figure out what is causing this. At this point I am not allowed to eat dairy to see if that will help me feel better. I also avoid most meats and fried food because they make me feel ill. I have no physical restrictions, but if I get hit in my stomach, I will throw up. I have been sick for 7 months now, and it is frustrating to live sick, but I am thankful beyond words that I am doing much better than I was 4 and 5 months ago.
1 Comment
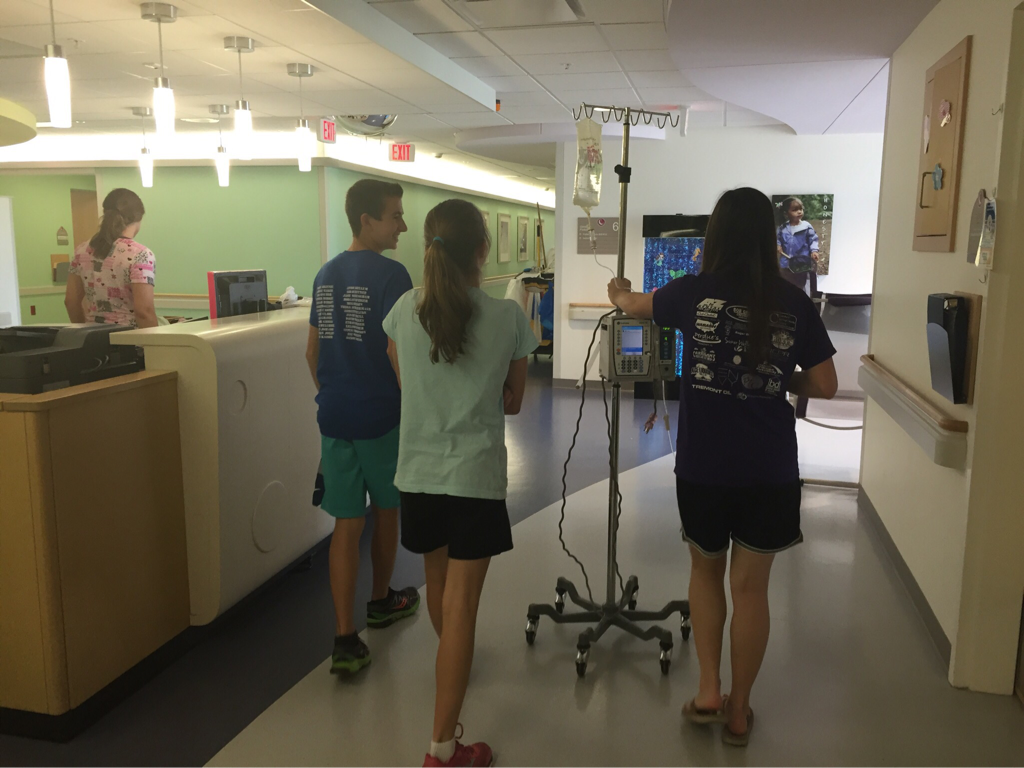
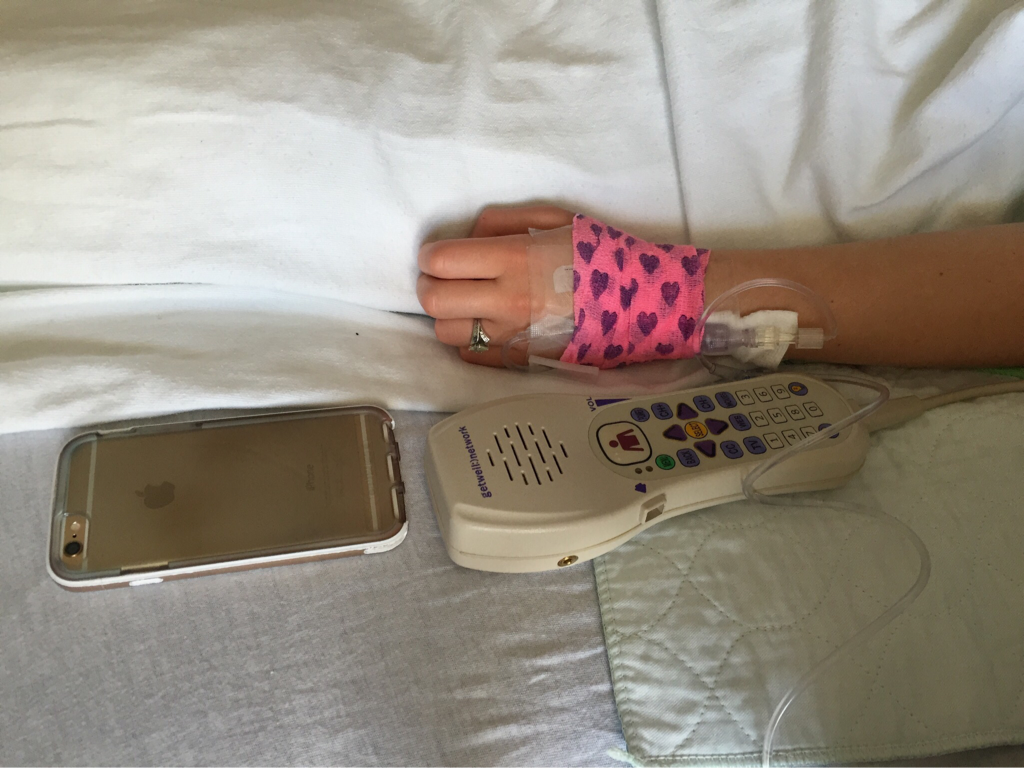
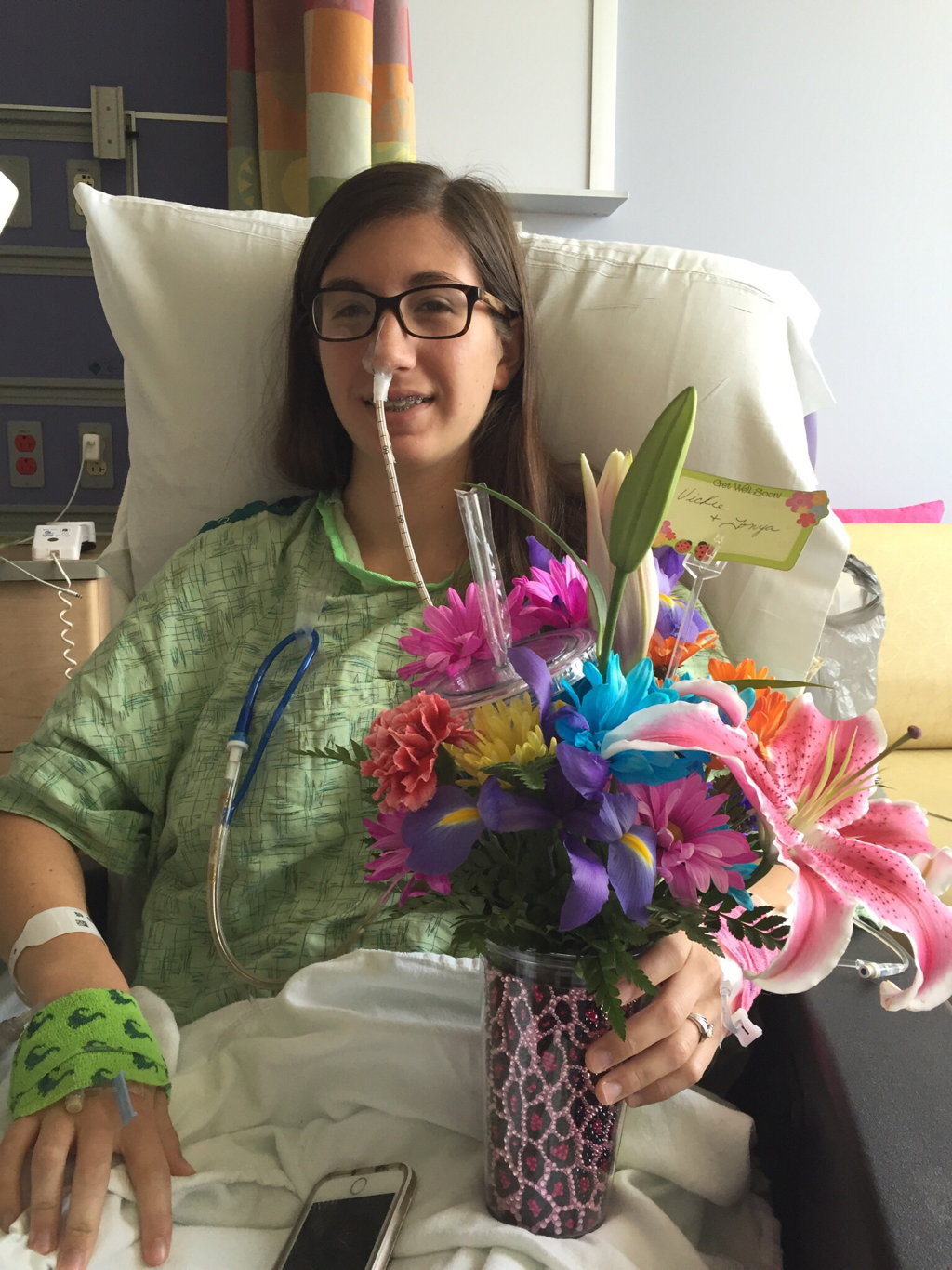
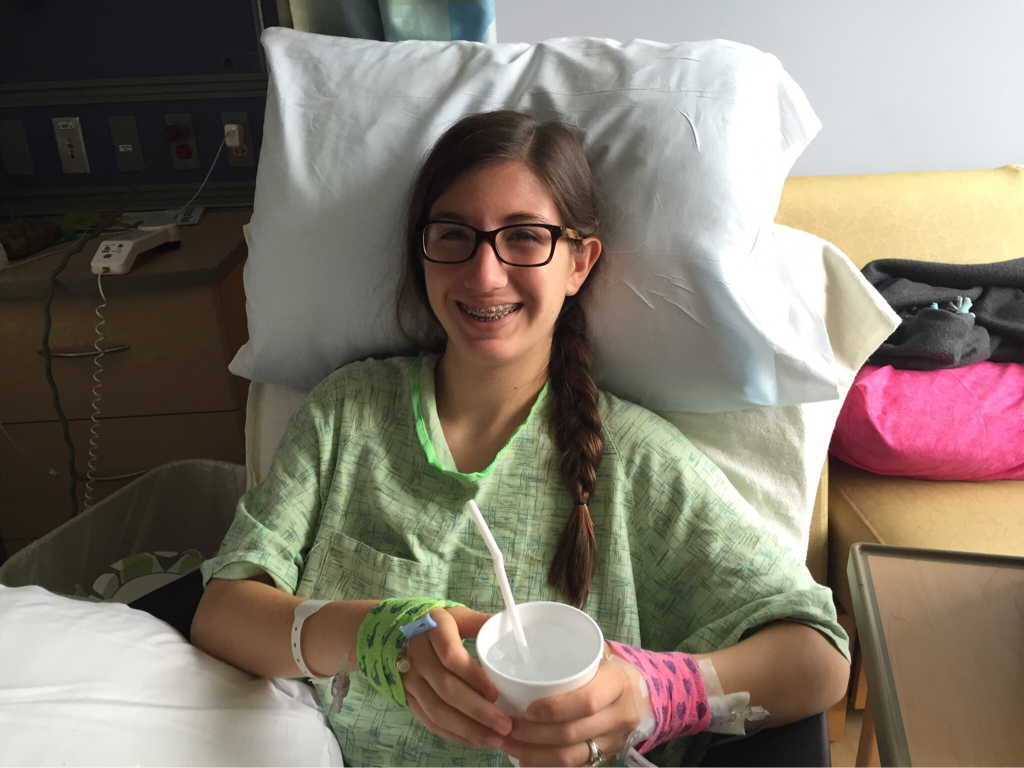
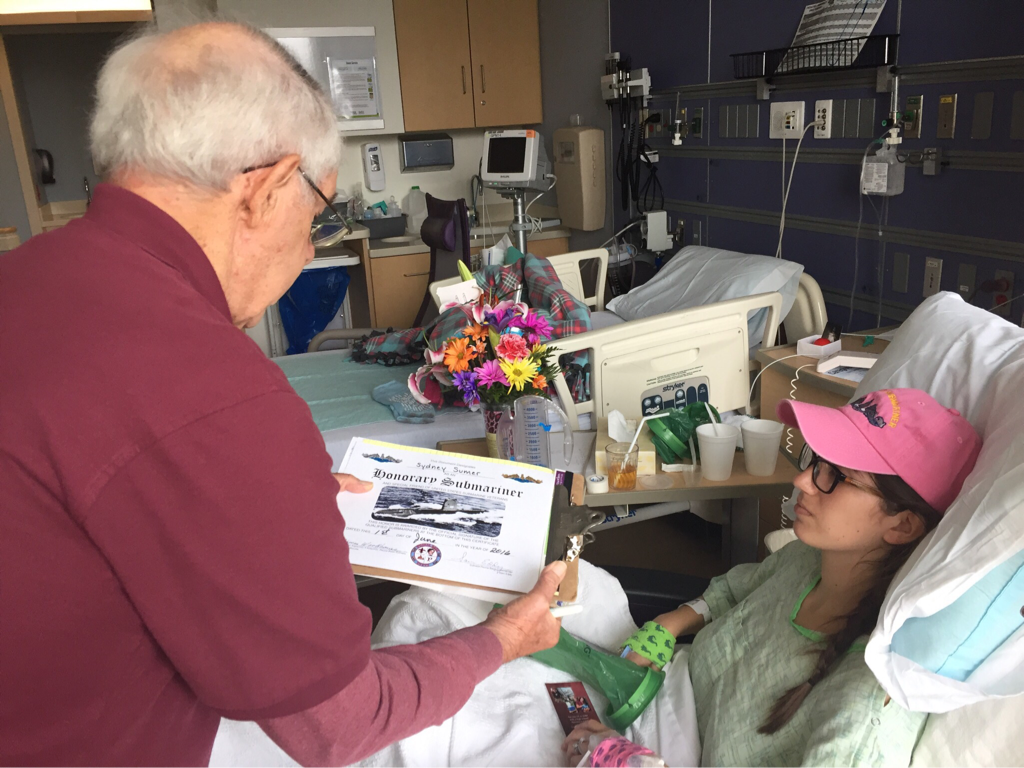
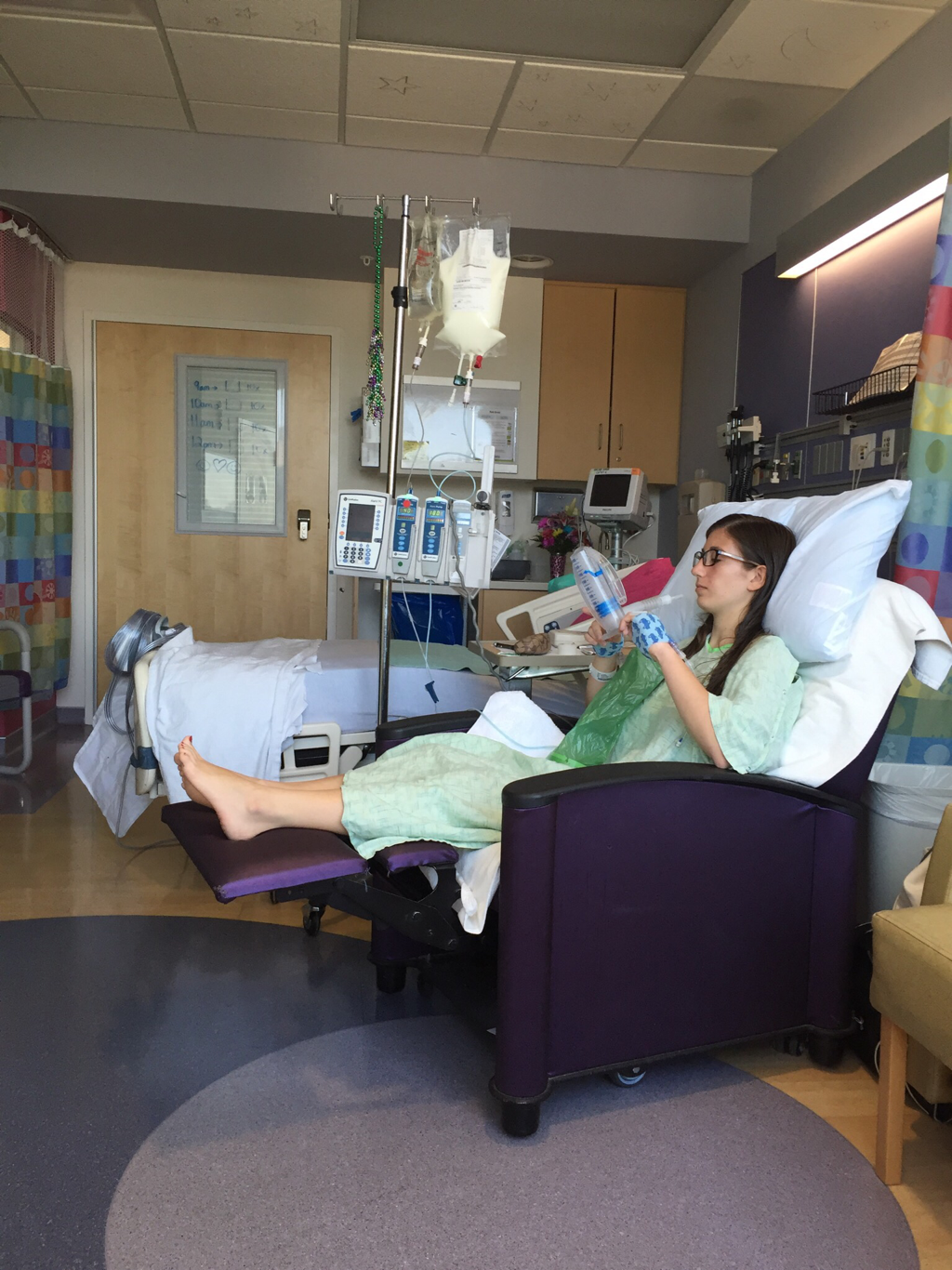
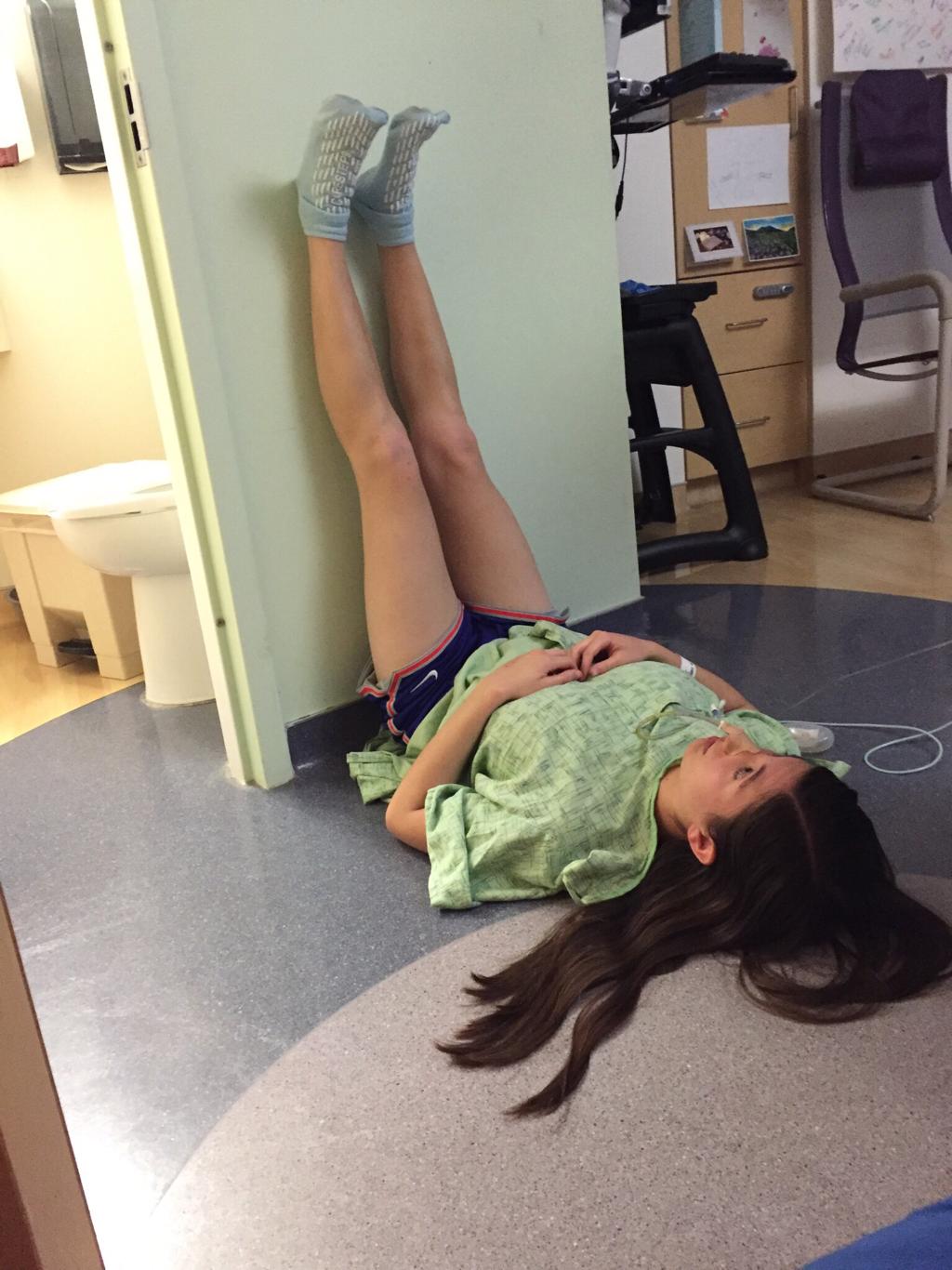
On July 22 I planned a visit to the hospital to see some of my nurses again and give them some treats, including cupcakes that I had made. It was such a great feeling to be able to give back to the nurses and PCTs and to be a visitor instead of a patient. They were thrilled to hear I was doing much better and recovering fairly well. They were also extremely ecstatic to find out I was no longer vomiting on a daily basis, which is a huge improvement for me! The staff at the children's hospital is awesome and because of them my stays were so much better! I can't thank everyone there enough for all they did while I was at the hospital! Since my discharge after my second hospital stay and third surgery, my recovery was going better than ever. I was only set back about a week and the bloating had gone down significantly. On Monday, July 25, I started to have abdominal and back pain again that prevented me from sleeping well that night. The pain slowly increased and I threw up Tuesday night. Wednesday morning I had a chiropractor appointment, and that helped my back for a few hours, but then Mom called the surgeons' clinic at the children's hospital. They had me come in asap for an abdominal x-ray and then later I saw one of the surgeons who was in clinic that afternoon. After looking at the x-rays and examining my abdomen, he determined that I was constipated. Thank goodness it wasn't an adhesion this time! I didn't think that I was constipated because I go to the bathroom regularly, over 50% of my diet is fruits and vegetables, and I take fiber supplements every day. He prescribed a suppository and I had to drink magnesium citrate that afternoon to try and clear me out. I also tried to drink lots of Gatorade and water in order to stay hydrated since I threw up Tuesday and clearing me out dehydrates me. I still didn't feel cleared out Thursday, so I drank a miralax bomb that day to help also. Except for some rice Wednesday night, I went 48 hours without holding any solids down because I felt nauseated and full. Now I'm eating again, but I'm very bloated and get full very easily. I've had to resort to ensure and boost drinks and Gatorade to make sure I'm getting enough calories to maintain my weight and have enough energy to make it through the day. Since my gut is malrotated, I'll have to deal with constipation long term and be especially careful for the next few months. I'll need to try and eat foods rich with fiber, and now I'm taking fiber supplements twice a day along with miralax once a day. Hopefully by doing that I'll be able to prevent major constipation issues and not have to clear myself out every couple weeks. I reached a huge milestone this past week by going on my first bike ride since last summer! I went 7 miles and stopped twice, but I made it! Before that the only physical activity I did was walk and stretch. My next goal for the near future is to start jogging and after that start lifting small weights to build up my endurance and strength. My recovery is frustrating at times because for the past six months, I haven't been able to go any longer than two weeks without some sort of set back. I feel like every time I take two steps forward I end up having to take a step backwards. The setbacks I have are more difficult to jump back from now because I'm still recovering versus if I were to have a setback when I have my full strength back. For example, if a "healthy" person were to get constipated, he or she may have to take a laxative daily and watch what they eat for only a few days, and then they'll be back to normal. For me, I get constipated while already watching my diet and taking fiber supplements which then cause me to go two days without eating. I try my best to stay hydrated after I get cleared out, have no energy, nap often for the next 2-3 days after I discover I'm constipated, and then slowly try to get back to eating a normal diet. Even though I'm often told that I look healthy, I've lost over 15% of my body weight and my gut still isn't working properly. I'm definitely looking forward to a time when I can feel and be as healthy as I look. I had another pain flare-up with vomiting Thursday, July 7, and went to the ER. It was my worst pain flare-up yet and caused me to vomit multiple times. I was admitted to the hospital and had a CT scan that showed a complete obstruction in my small intestine. I was throwing up bile and gastric fluids again, so I had an ng-tube put in while I was awake to try and help me keep down some of the contrast for the CT scan. It didn't work, and the ng-tube was removed shortly after finding out the results of the CT scan. I ended up having emergency surgery Friday night. Dr. Yang was not the doctor on call Friday night, so another doctor, Dr. Bob Kanard, did my surgery. The doctors were not sure if they were going to find something as simple as an adhesion or something as complex as part of my bowel being dead. Thankfully, I ended up having an adhesion that was causing my problem. Because of the adhesion, the surgery I had was a diagnostic laparoscopy with lysis of adhesions. Part of my small intestine was stuck to the abdominal wall behind my belly button which caused my intestine to twist. The bowel was not looking too healthy, but once the surgeon cut the adhesion, my intestine untwisted and pinked up, which fixed the problem, and now I'm recovering. He did not have to put in an ng-tube in, so after the surgery I was tube free! I was able to use the bathroom with minimal help just hours after my surgery. Saturday morning I was allowed to try liquids, and by Saturday evening I was able to eat some chicken noodle soup! This was definitely the easiest recovery of all three surgeries! I was discharged Sunday morning and except for not being allowed to swim in lakes or rivers for two weeks, I have no restrictions and can continue to recover. Since being discharged, with the exception of a little pain at the incision sites, I am back on track for my recovery. I'm eating the same as I was before my third surgery, and I was only set back about a week. Also, since the third surgery my bloating has gone down a considerable amount, and my belly button looks somewhat normal again! This post is purely photos taken during and shortly after my hospital stay. They are all posted in the order they were taken. Some of them really make me reflect upon how far I've come since my surgeries. Because of my conviction to stay modest, I will not post any pictures of my stomach. I have seven total incisions between the two surgeries, and at one point I had a loop drain in my belly button and a jp-drain just to the left of it (on my right side). Photographs can speak a thousand words, and I think they depict my journey better than words could ever describe. 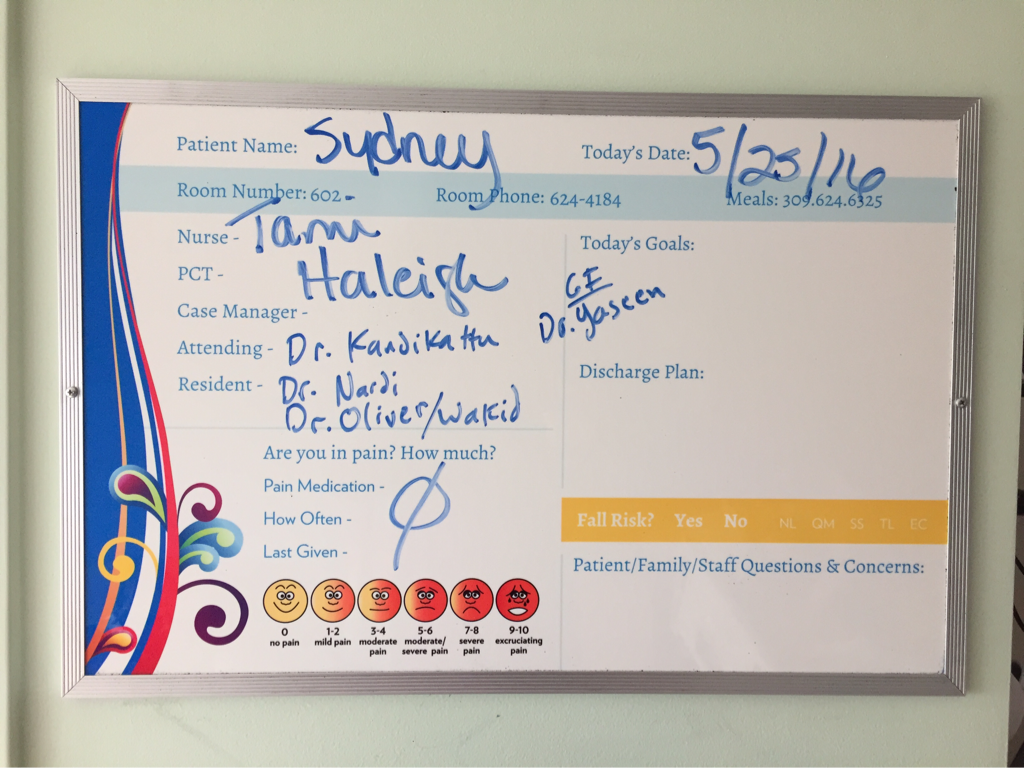 May 25 - This board was updated every shift change and whenever else it was needed, and it showed what medicines I was taking when, how much pain I was in, and who my nurse or patient care technician was. A day or two after this picture was taken all my doctors were changed to the surgeon team instead of the general pediatrics team. 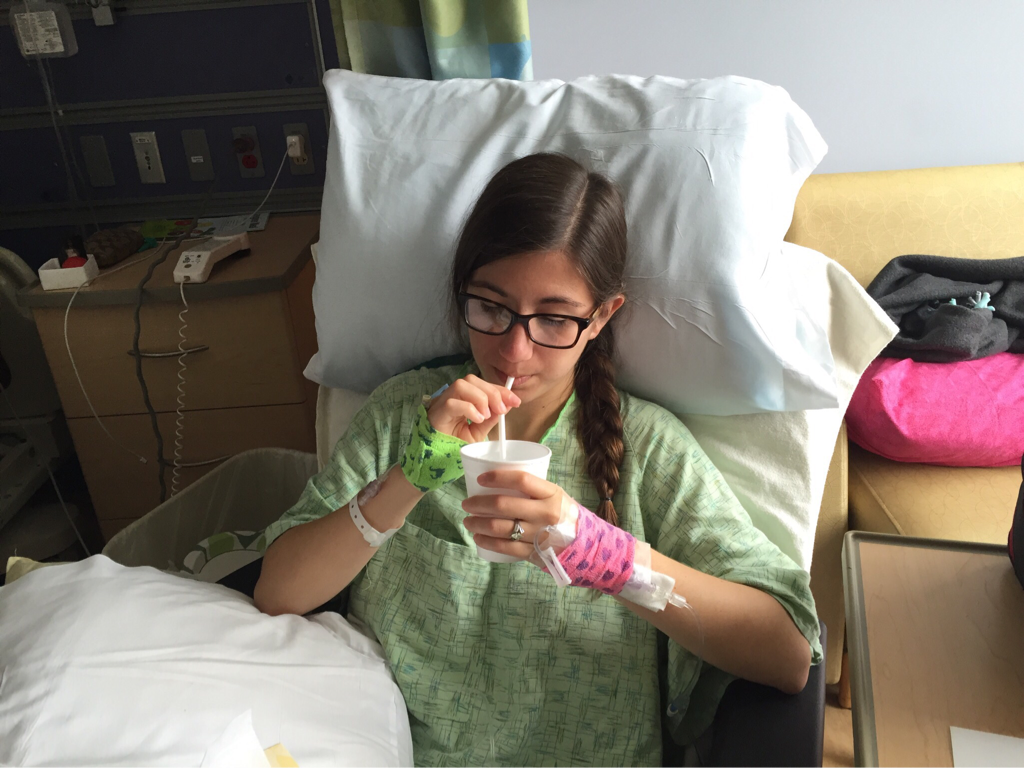 May 31 - My ng-tube was removed that morning. There was less bile and gastric fluid being suctioned out each day, so the doctors thought I was ready for it to be removed. That evening after having some chicken broth and jello I began to throw up liters of bile and gastric fluids. It was later discovered that I had a complete obstruction, so I kept throwing up liters of that green fluid until my second surgery. 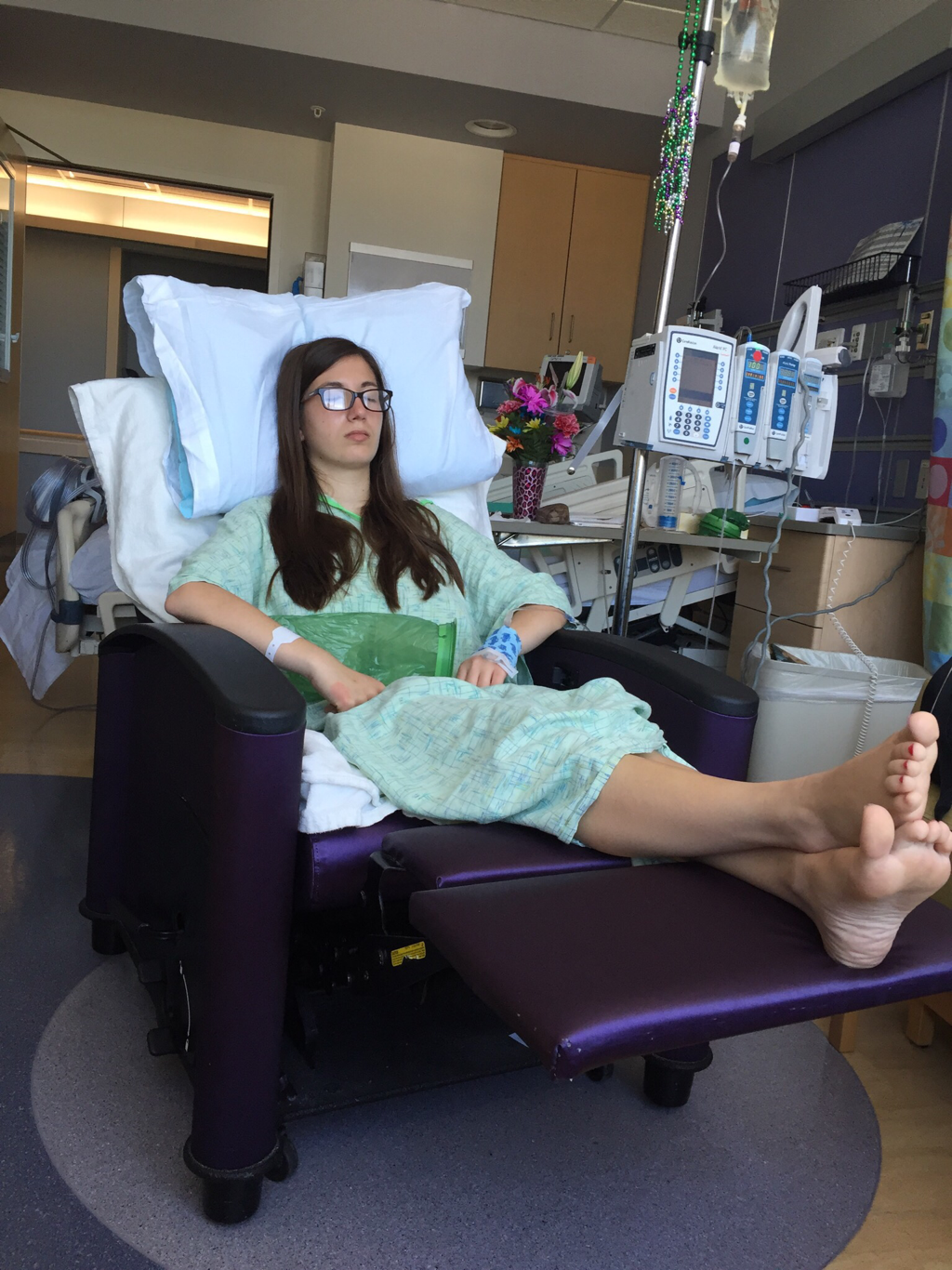 June 2 - I was feeling pretty miserable that day. Every few hours I would throw up even though I wasn't eating or drinking anything. It was difficult to sleep because I was constantly throwing up and feeling nauseated. June 2 was also a very difficult day because we discovered that I was going to need a second surgery. 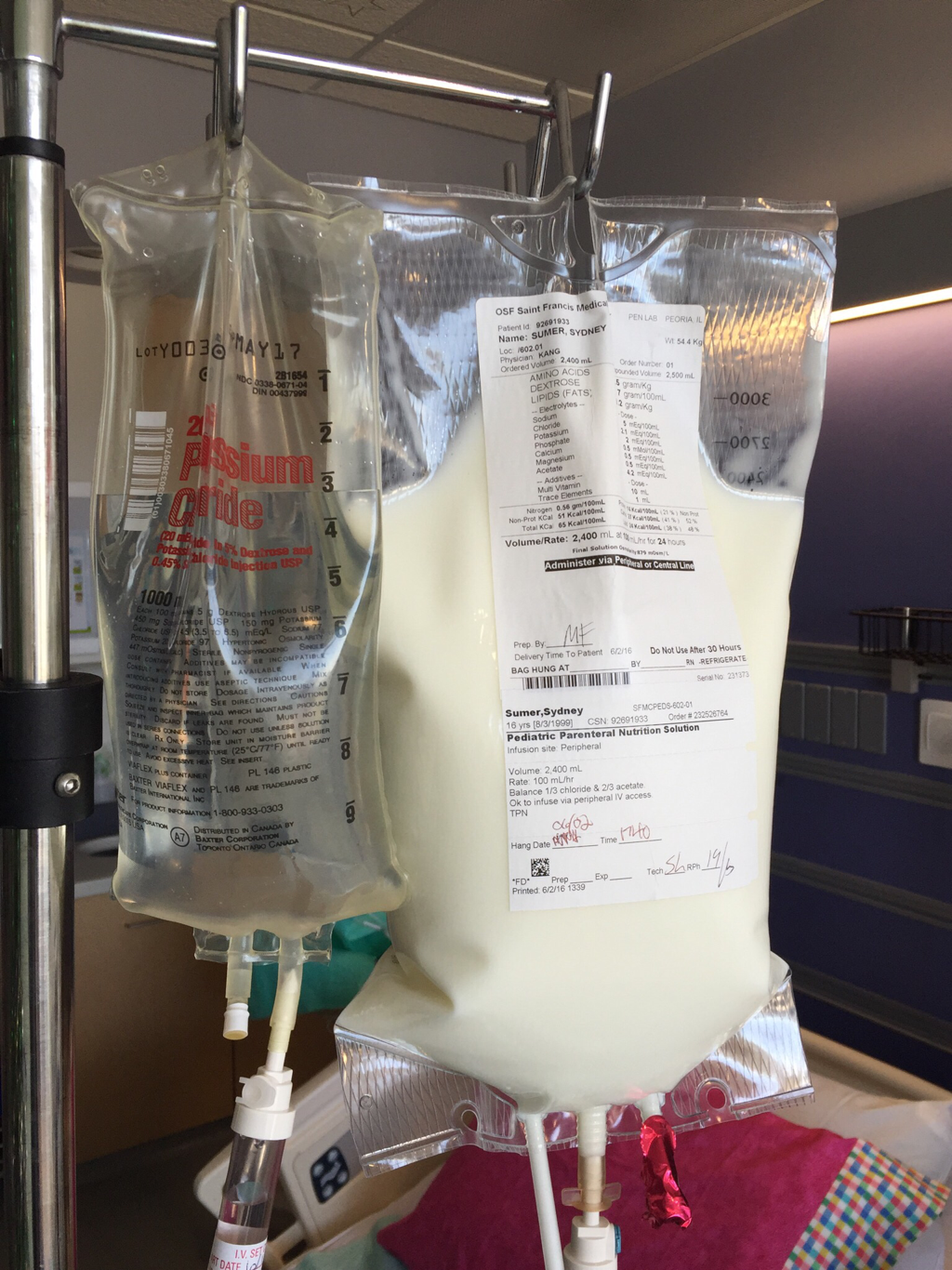 June 2 - That evening I was started on Pediatric Parenteral Nutrition (PPN). With the exception of about six ounces of chicken broth, I hadn't had anything to eat or drink since May 26, which was exactly a week without nutrition. This temporarily went into an IV in my right hand but after 24 hours was moved to the jugular IV that was put in place during my second surgery. 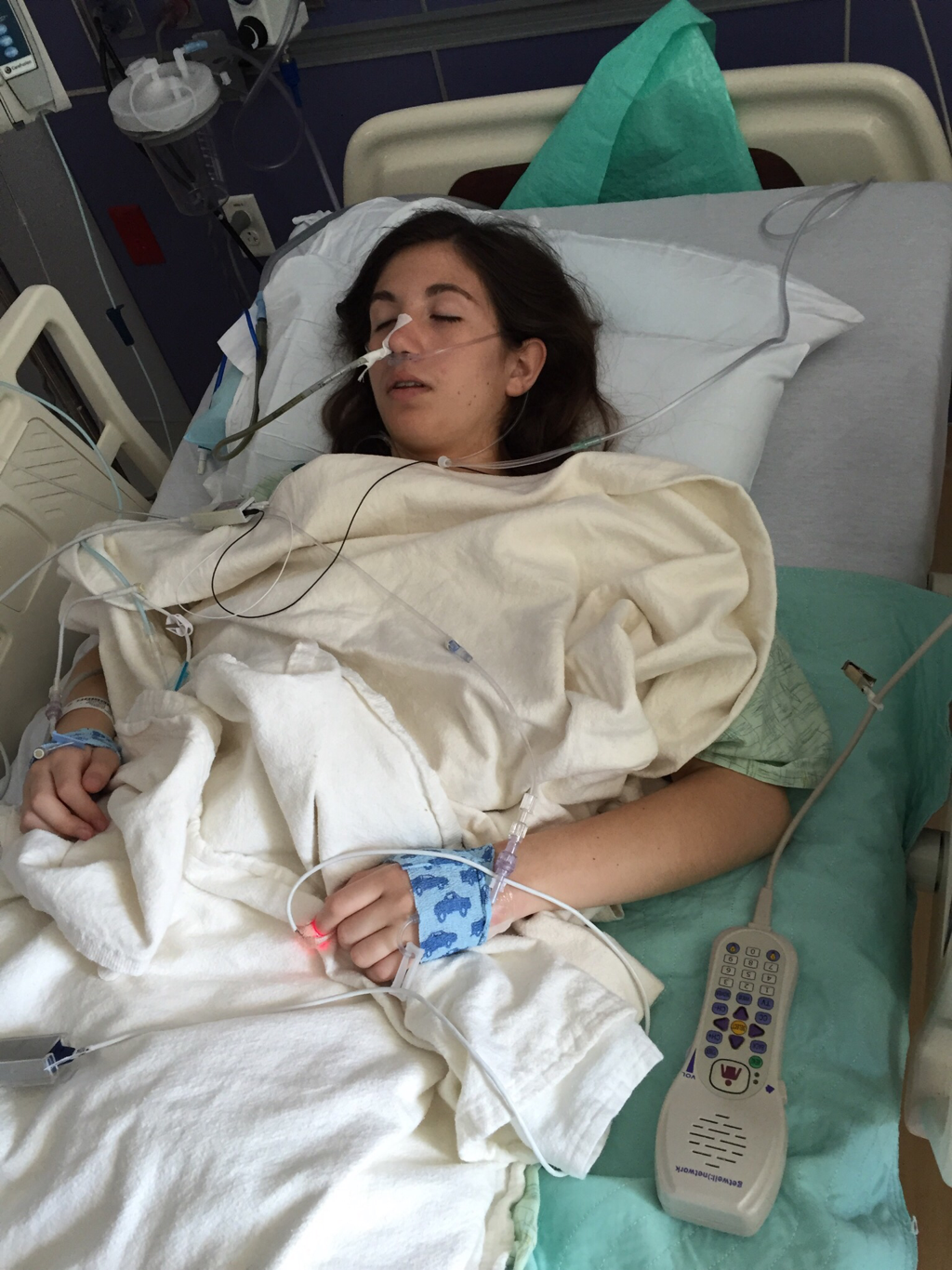 June 3 - This picture was taken a couple of hours after my second surgery. Honestly, it scares me and really makes me thankful for all that I've overcome. I debated whether or not I should post this picture for a while, but I decided to post it to show that this is reality. It's real life. In the picture I had an ng-tube in my nose that was connected to a canister that suctioned fluid from my stomach, oxygen, three leads on my chest and side that were connected to a monitor, a pulsox on my left index finger, IV fluids going into my left hand, PPN going into my right hand, an IV in my neck, a jp-tube in my abdomen that was suctioning out fluid from the incision on my duodenum, and a loop drain in my belly button. Later that evening both the IV fluids and PPN were moved from my hands to the jugular IV in my neck. 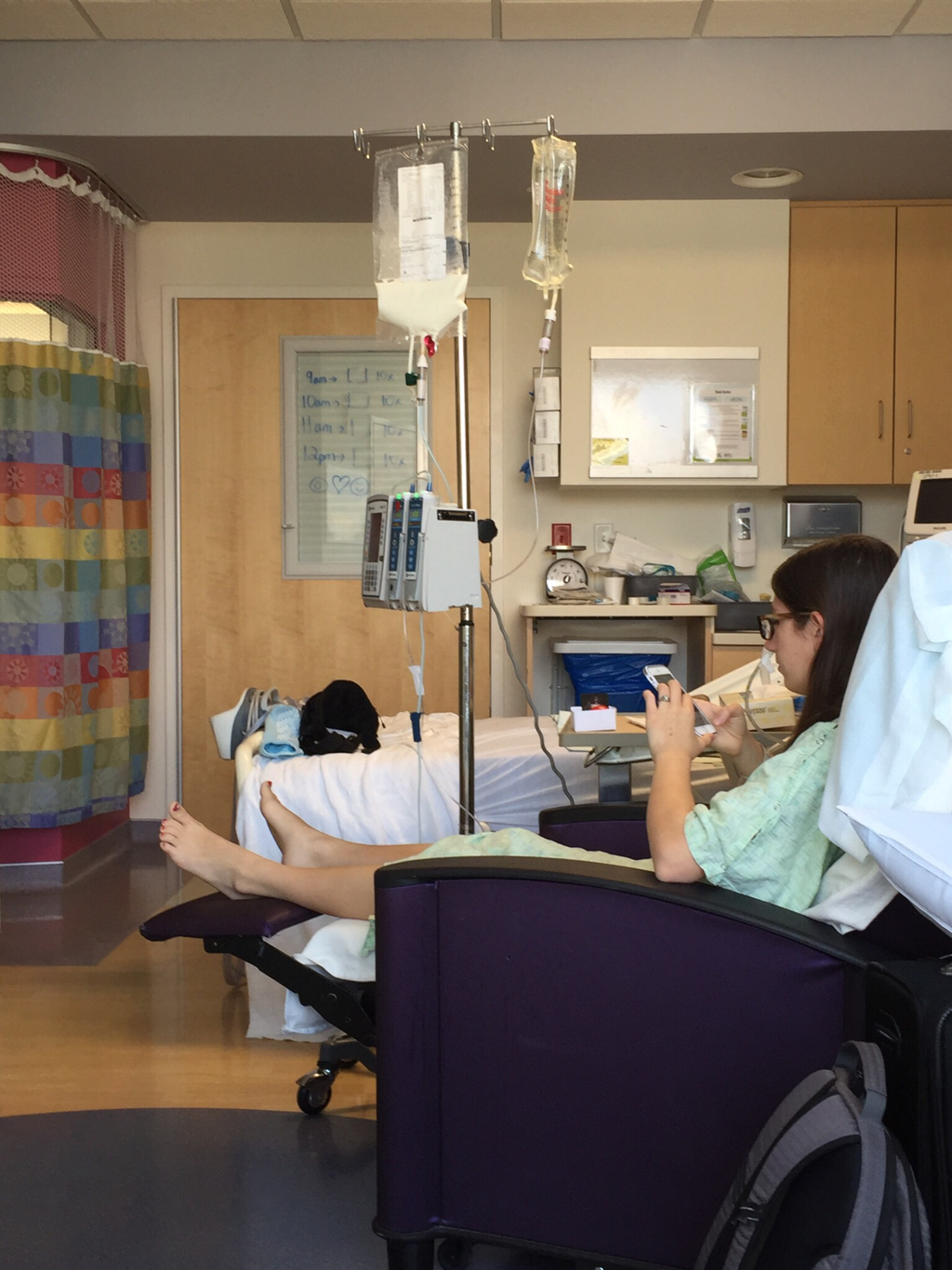 June 4 - This is the day after my second surgery. My recover for this surgery was much easier at the beginning because it initially only took two people to get me out of bed and I was able to sit in the chair much easier. In the background, there is a black fanny-pack on my bed. I used that to hold my jp-drain in when I went on walks. Next to it are the light blue hospital socks I wore.  June 7 - This was my first time outside since I had been admitted. I was not strong enough to walk all the way outside, but once I was outside I was able to walk a bit. We found a semi-private area to go because people would stare a lot. I'm blowing my nose because my ng-tune was recently pulled out 5 cm, and my nose would not stop running and I was very congested. 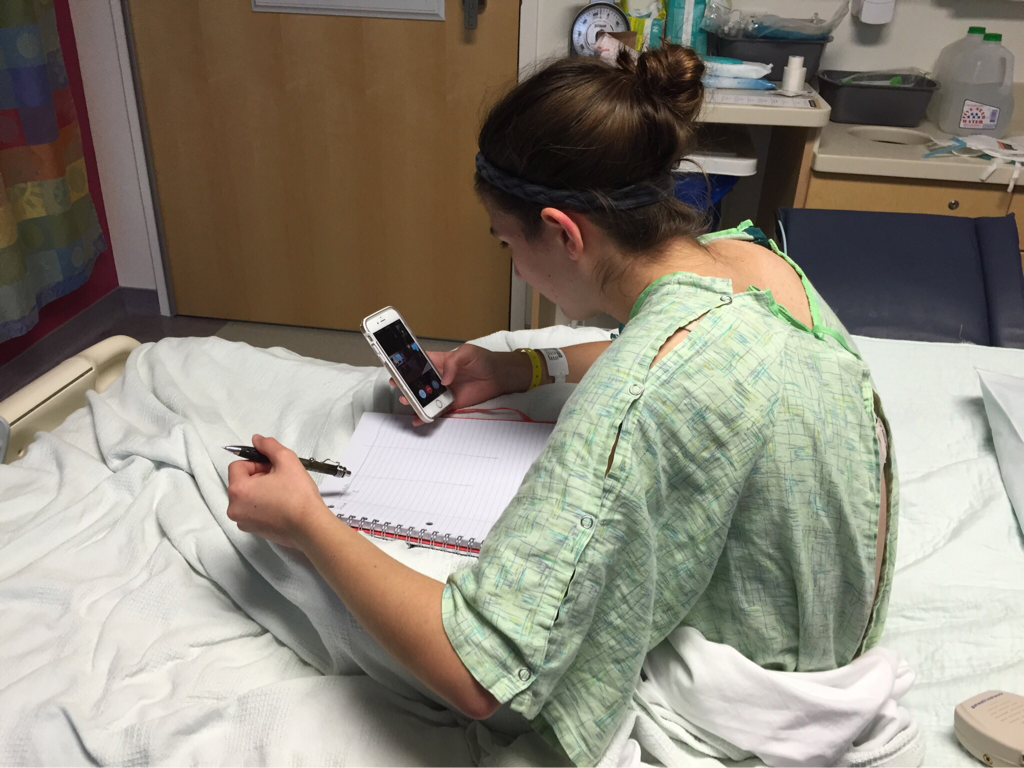 June 11 - I missed out on The Cabin, which is a youth group for high school and college aged kids. I was able to FaceTime one of my friends and help judge the mangeant (man pageant), which was the theme for the night. I had just thrown up about half an hour earlier, so being a part of The Cabin at the hospital really lifted my spirits. I had my first post-op doctors appointment with my surgeon, Dr. Yang, last Tuesday, June 28. At the appointment I discovered that I have been maintaining the weight I had at my discharge, which is a huge step forward for me. All of my restrictions are lifted, but I am continuing on my medicines for another two months. One medicine promotes stomach motility and the other reduces stomach acid/inflammation. I will have a follow-up appointment with another surgeon in two months because Dr. Yang is leaving The Children's Hospital of Illinois on July 15. Dr. Yang told me, "You have no restrictions now, but it's up to you to fight through the pain." He also said that it will probably be six months to a year before I'm back to "normal". I also do not have any dietary restrictions, but for right now I do not eat normal sized meals, more than a few bites of meats, or greasy/fried foods. Right now my stomach is bloated, and it becomes even more bloated after I eat or drink something. Dr. Yang ordered some x-rays because he suspected that the bloating could be caused by constipation. The x-rays showed some mild constipation but nothing major, so I'll be taking extra fiber for at least the next few months. The constipation may be temporary, or it may be something I'll have to deal with in the long run since my gut is malrotated. But hey, I'd rather be constipated than be starving to death, so this is definitely an improvement. Every few days I also get pain flare-ups and up until lately, not even ibuprofen or tylenol would take an edge off of the pain. The flare-ups are most likely caused by scar tissue, and will hopefully subside over time. I also most likely still have gastroparesis because after I eat, I feel full for a while afterwards. Also, I have yet to feel hungry. In time maybe I'll feel hungry again. In a little while Dad said that would like to have another motility test done to see if I still have gastroparesis and if I do, to see how bad it is.
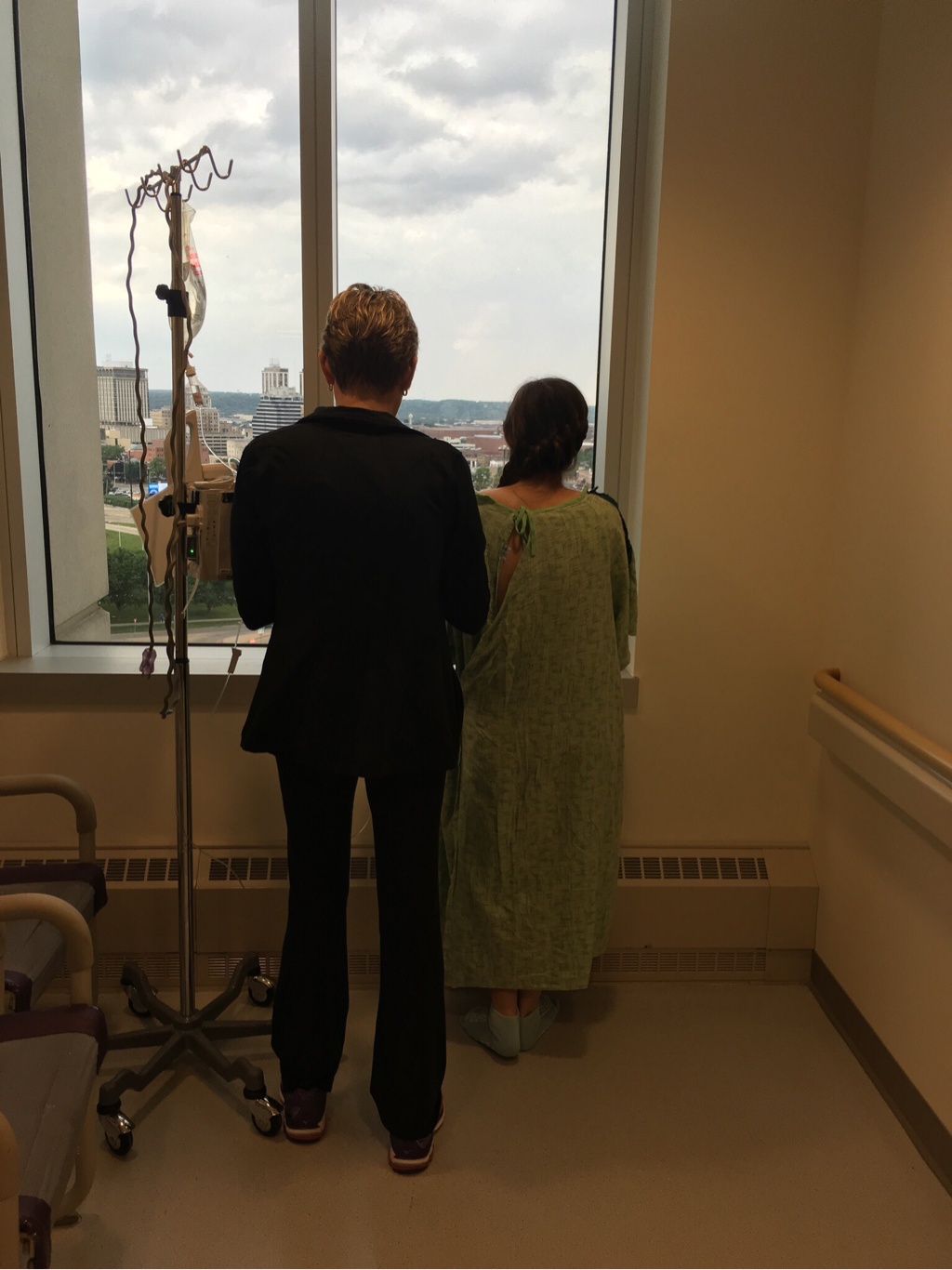
Because I had such extensive surgeries, I'm anticipating having to be careful about what I eat for the rest of my life. I'll have to be careful to not overeat, not eat anything that could potentially cause pain due to being too heavy or hard to digest, and make sure to eat lots of fiber and protein. I'm also anticipating having do deal with random, but hopefully not frequent, flare-ups of pain due to scar tissue and adhesions. One last note, as of yesterday, I have officially not thrown up in over 2 weeks. The last time I did that was 5 months ago. I'm getting better slowly but surely! I'm home!!! I finally got discharged on Tuesday, June 14, after spending exactly 3 weeks in the hospital. The jugular IV was removed that morning and by 2:00 p.m. I was home! The first thing I did when I got home was greet Biscuit (the dog) and then take an extremely long and very much needed shower. Then I decided to surprise a few of my friends by not telling them I was discharged and showing up at their houses. It was pretty great! It is a huge relief to be home. I no longer have my vitals checked every four hours, and I get to sleep in my own bed! When I was in the hospital, there was a lot less pressure put on me when I ate. If I were to throw up, that would be at least one more day I would have to stay. In order to be discharged, I had to be able to use the bathroom and hold down enough water and food to sustain myself all without throwing up. Now I don't have that weight on my shoulders anymore, but it still is best if I didn't throw up. For at least the first two weeks after being discharged, I have a lot of restrictions. Some of them include not being able to go to school, ride my bike, or lift anything greater than 5 pounds. My recovery is going okay, but I'm still eating a fairly bland diet with easily digestible and high calorie foods. I still have to be careful with what I eat though, because I think I might have overdone it Sunday, and I threw up just after midnight on Monday. Throwing up every so often is to be expected as my body adjusts to eating and digesting food again. I went 9 days without throwing up, and for me, that's pretty impressive. My low back pain and stomach pain prevent me from sleeping well, but I have started seeing a chiropractor, and his adjustments are helping with the pain. It was also discovered that I have mild scoliosis - my left hip is higher than my right hip - and slight kyphosis, but those can be helped and potentially reversed with regular adjustments. Right now I weigh less than I have at any other point during my illness. I weigh the same as I did in seventh grade, which was four years ago. I'm struggling to find clothes that fit properly because my stomach is very bloated. My waist is a size bigger than the rest of my body, so a decent amount of the clothes I wear now, I wore back in middle school... I'm also too tired to go shopping. I tried a few days ago with my mom, but I barely made it through three stores with rests in between. I also had no success in those stores. Maybe for now I should stick with online shopping. Today I made the front page of the Peoria Journal Star. The day before I got discharged a lady at the hospital asked if it would be okay for me to be interviewed for an article to go with a recent sleep study, and I agreed. The photographer and journalist spent 45 minutes in my room taking pictures of the nurses and me and asking me questions about what it is like to sleep in a hospital and how often I get woken up by the nurses. Here is the link to that article: http://www.pjstar.com/news/20160620/childrens-hospital-of-illinois-is-on-leading-edge-of-integrating-sleep-into-health-care Two days ago I ate my first food since May 25. I was definitely excited to take another step forward, but that excitement did not last long. Not even an hour after eating my few bites of egg, biscuit, and applesauce, I threw up. Almost immediately after I ate, physical therapy came in to work on exercises to strengthen my core and back, and that may have attributed to the vomting. I also have to remember that my stomach is not used to working. Not only did I have two major surgeries, but my stomach has not been working properly since the beginning of February. It will take a while for it to start working, and I must be patient. Both yesterday and the day before I threw up about 1 liter of gastric fluids at around 7:00 p.m. The doctor did not seem to be worried and said that it will take a while for me to start holding down food, and the amount I threw up is still less than what was previously being suctioned by my ng-tube, so that is a good sign. Whenever I eat, I try to walk and then lay on my right side because that is how fluids passed through my stomach and duodenum the best when I had the upper GI performed. The thought is that laying on my right side will allow food to digest easier, and walking promotes motility. I have been experiencing nausea and have to mentally fight in order to not throw up my food. I literally beg to God to let the food pass because I dearly want to go home and be able to hold down food without pain or nausea. Eating makes me really uncomfortable and at this point I am hesitant to even try the smallest amounts of food. A friend of mine got married on June 10, and I was very bummed when I discovered that I would not be able to attend the wedding. To my surprise, one of my friends visiting earlier that day suggested that maybe I could FaceTime him and watch the wedding. Sure enough, at 6:35 that evening I got a FaceTime call and was able to watch the entire wedding! I was also able to mute my side so I would not disturb the ceremony. It was totally unexpected but it was an awesome experience. It is probably a good thing I was not able to attend the wedding because I had to hand my phone off to my dad at one point while I threw up... On Sarurday the 11th, I was going to miss the Cabin. The Cabin is a sort of youth group for high school and college aged kids on Saturday nights. The theme for that night was mangeant (man pageant) to imitate the Turkey Festival. Another one of my friends offered to FaceTime me so I could watch the mangeant, and I even ended up being one of the judges! It totally made my night because I had been disappointed about half an hour earlier by a bout of puke. Not only did I get to FaceTime for the mangeant, but one of the parents in charge of the Cabin decided to video tape the mangeant and the speaker, so hopefully I can watch that videos soon! So far, today has been the best day so far. I started a medicine that promotes stomach motility, and I think it is helping. I held down a breakfast of half a piece of toast, apple juice, and some applesauce. I also held down my lunch and dinner, which consisted of a fruit smoothie Mom made and brought from home and some organic graham crackers. They were definitely better than hospital food! I have yet to throw up today, and hopefully I can keep it that way. As soon as I can hold down enough food to sustain myself and not throw up, then I can can get the jugular IV removed - it's giving me TPN - and go home. That would be awesome, but it still may take a while. Today marks 16 days in the hospital. On June 7 I was given permission to leave the floor. For the first time in two weeks I went outside. It was absolutely gorgeous, my family and I found a little courtyard with an empty pond that was fairly private, and I was able to walk when I was outside too. My recovery has been a roller coaster of good and bad, but as far as my physical strength goes I've been improving little by little every day. Since the second surgery I had been experiencing low back pain from both laying in bed for extended periods of time and from overusing my back muscles because my stomach muscles were extremely weak. A physical therapist started helping me by giving me exercises and a TENS unit to help relax my back. I can now walk multiple laps around the floor, sit up, stand up, and do physical therapy exercises/stretches, all with no assistance.
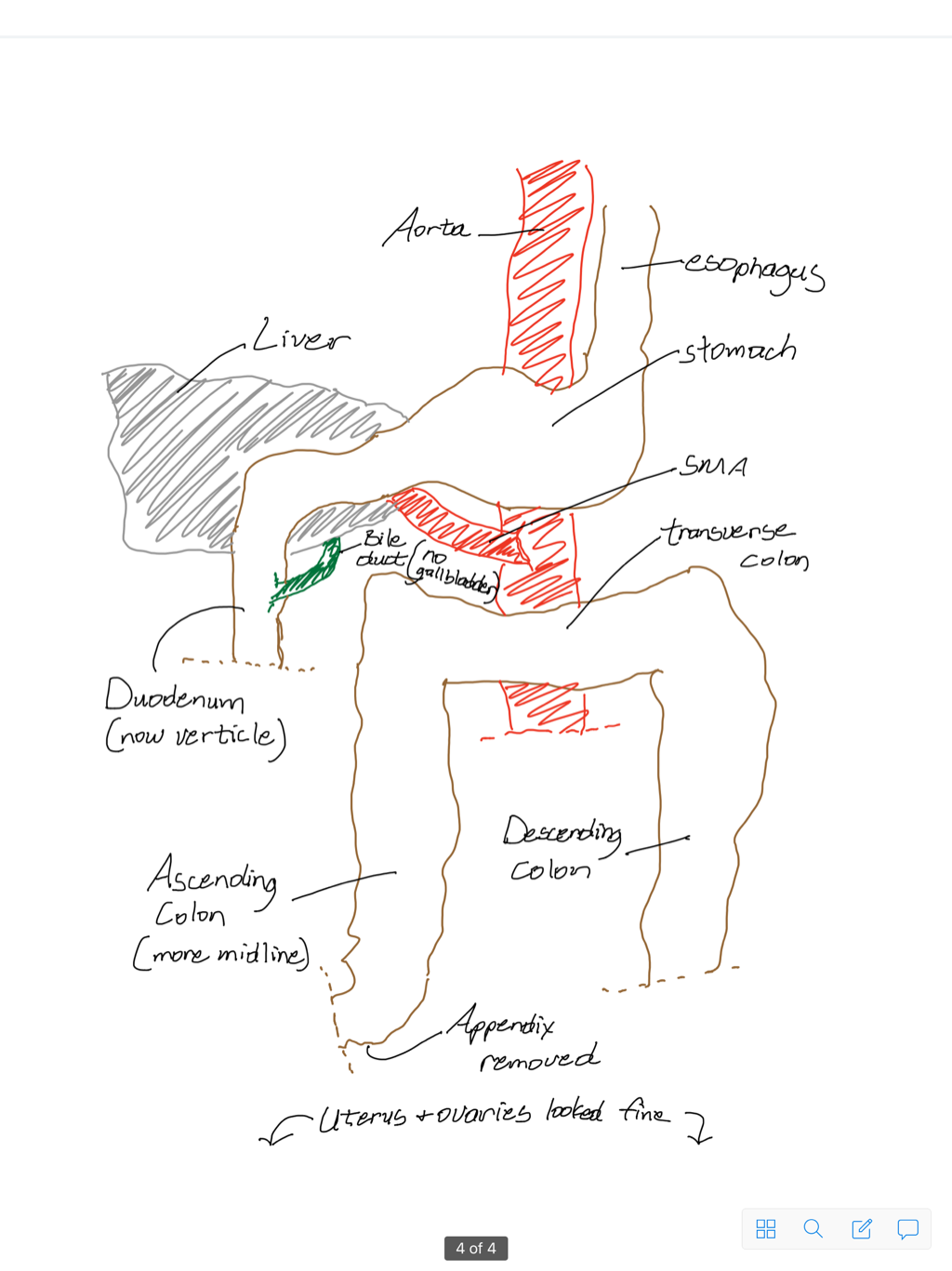
Since the second surgery, I had been having a lot of output from my ng-tube. Every 12 hours about 1000 cc (1 liter) of bile and stomach juices were suctioned out of my stomach. That is a lot because the stomach normally makes 1 1/2 to 2 liters of fluid a day. On the afternoon of June 7, Dr. Yang came in and prepared us for the potential of a third (and non-laparoscopic) surgery or different long-term options like tubes to feed me and suction my stomach simultaneously. We were all very scared and there were a lot of visitors that night and a lot of people praying too. At 8:00 a.m. on June 8, I had another upper GI and the contrast went through my duodenum without difficulty. I have no physical obstruction and it is truly a miracle! Every doctor, resident, and surgeon my family talked to believed that with the amount of output coming from my ng-tube, I would have a definite obstruction. Now it is believed that I just have gastroparesis, - most likely post-op - so my stomach and duodenum are just slow to work. But again, THERE IS NO OBSTRUCTION!!! Prayer is more powerful then I could ever imagine!!! Because of the great results from the upper GI, both the jp-drain in my stomach and loop-drain in my belly button were removed later that afternoon. My ng-tube was clamped for the upper GI, and it remained off of suction until 10:00 p.m., and I experienced no nausea. This morning when the doctors did their rounds, they removed the ng-tube! Then, this afternoon I was given the order to be allowed to have sips of clear liquids! So far I've had about 10 oz of apple juice and seem to be doing well. Hopefully it will stay down and I can keep moving forward tomorrowand the next day! Thank you to everyone who has stopped by and visited or sent encouraging texts or cards! All of it helps my hospital stay be more bearable, and knowing that people out there are praying for me is priceless! For the surgery on May 27, the surgeon ended up doing a Ladd's procedure where he essentially repositioned my duodenum and colon. He cut the ligament of Treitz, so my duodenum goes straight down. Then, my duodenum was overlapping my ascending colon, so he mal-rotated my colon towards the center of my abdomen. No cutting of my bowels was necessary, but the tissue behind my ascending colon was dissected in order to move my colon, which made this an extensive procedure. By doing the Ladd's procedure, he had to remove my appendix because it was relocated when my colon was moved, and if I were to get appendicitis in the future, it would be difficult to diagnose and remove the appendix. They also removed my gallbladder, which they later found to be cholecystitis (inflamed and irritated). Everything was done laparoscopically and I have five small incisions. Both that night and the next day I experienced a bout of extreme pain in my chest and lungs as the air pumped into my abdomen during surgery moved up into my diaphragm and shoulders and made it difficult to breathe. I also lost feeling in my arms and legs for about an hour and a half due to lack of oxygen circulation. After being put on oxygen and given more pain medicine I was able to control the pain in my chest and shoulders. I had an ng-tube put down my nose and into my stomach during surgery to suction out bile and such from my stomach. That was removed the morning of May 31. The past couple days I had been allowed to eat some ice chips and suck on hard candy. I was able to start on some liquids that day. My pain had gone down quite a bit and I took a few walks a day and had been able to sit in a chair since the 30th. I thought I would be at the hospital at least through Wednesday (the 1st) as the doctors wanted to make sure my stomach and intestines work before I get to go home. Later that day after having some chicken broth and jello, I began to feel nauseated and started throwing up. I was throwing up much more than I had consumed and the vomit looked like the stuff that had previously been suctioned out of my ng-tube. The vomiting continued through June 2. On June 2, the doctors ordered an upper GI (I drank barium and x-rays were taken), and it was discovered that my duodenum was completely obstructed. There was some sort of kink and nothing was getting through. On June 3, I went in for an EGD to see from the inside what may be causing the obstruction. A kink was discovered, but the camera was able to be pushed through the kink. The EGD preceded another laparoscopic procedure to correct the kink. The surgeon discovered a stricture and the kink in my duodenum by going in surgically. There was a stricture that was either caused by the SMA previously constricting my duodenum or from my duodenum kinking after the first surgery. The surgeon cut through some scar tissue (that was caused by the stricture) and sewed my duodenum back together in a procedure called a duodenal stricturoplasty. I also got an IV put in my neck to give me TPN (nutrition), another ng-tube for suction again, and a tube in my stomach wall that suctions out the excess fluid by my duodenum. That tube in my stomach makes a 6th incision in my abdomen. My recovery in the hospital will probably take a week. So far my recovery from this surgery has been easier than the recovery from my first surgery. I have not experienced the chest pain, and I was able to use the bathroom fairly easily and have even begun walking and sitting again. The doctors will be very cautious about removing the ng-tube and the tube in my abdomen so that there is no pressure on my incision site. I was told I could eat a few ice chips today, for comfort, and hopefully over the next few days the ng-tube will be clamped and I will be able to hold down liquids. Here is a lot of information about what has happened these past couple days and what the plan is for the future. I apologize for those of you who do not understand all of the medical terminology, but I will try to explain it to the best of my abilities.
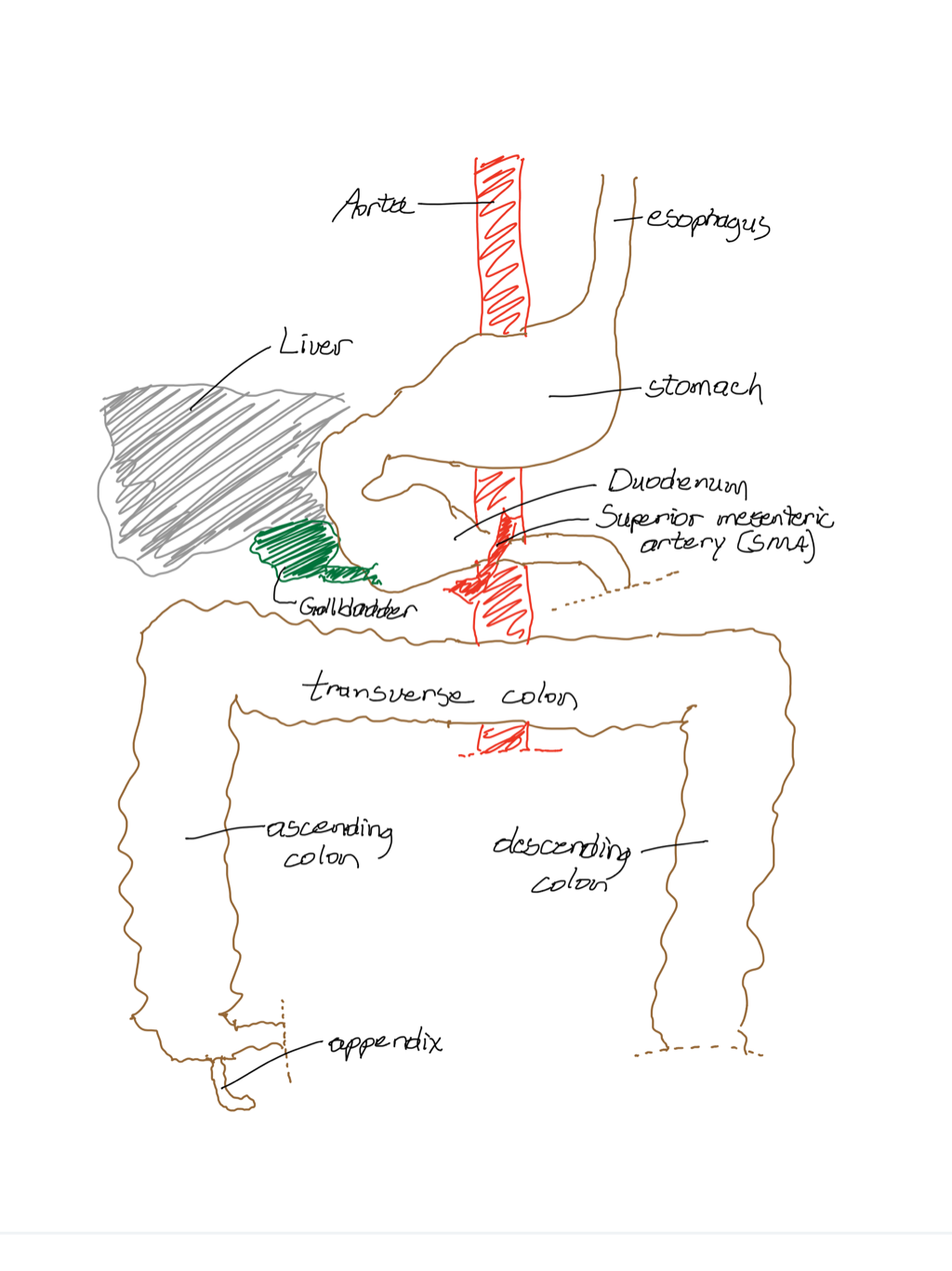
On Wednesday I was admitted to the hospital (OSF Children's Hospital in Peoria, IL) by my pediatric GI, Dr. Mohammad Yaseen. It was kind of unexpected, but he wanted to get me on IV fluids and possibly do a repeat EGD and insert an NJ tube at the same time. Since yesterday, we have talked to various doctors about the possibilities of various feeding tubes and potential surgery. The plan is for Dr. Edmund Yang to perform the surgery tomorrow morning. The doctors and my family have discussed various treatment options and places to be treated and decided this would be the best route to take. My dad is a DO and runs a family medical practice in Pekin, IL, and my mom is a non-practicing PA-C, so my family has experience in the medical realm. We have researched further into SMA syndrome and other possible diagnoses and discussed whether or not it would be better to to go to the Mayo clinic in Minnesota or to another research based college/hospital. Through that research and talking to various doctors and surgeons, we believe that despite the rarity of SMA syndrome, this hospital is equipped to treat it, and Dr. Yang has some experience with SMA syndrome, has performed surgeries similar to a duodenojejunostomy, and is reputed to be a very good surgeon by other surgeons, hospitalists, and Dr. Yaseen. To begin explaining SMA syndrome, the angle of my aorta and superior mesenteric artery (SMA) is 8 degrees. We considered having a feeding tube to try and increase my fat pad (which in turn would increase the angle between the aorta and SMA). Chances are if the feeding tube did work, it would only work temporarily because if I were to return to the active lifestyle I once had, any minor weight loss could cause me to become sick again. Also, it is now believed that the small angle is congenital - which means it's been like that since birth but has only been noticed since I got sick in the beginning of February - so gaining weight would have little effect. Dr. Yang is also going to remove my gallbladder. I had a HIDA scan done back in April and it showed normal function (54%), but when my gallbladder would pump food from my stomach into my intestines, bile would come back up. Also, when injected with the hormone that makes my gallbladder contract, I experienced an increase in pain, which could mean that the gallbladder is not functioning as it should. The doctors believe that both the SMA syndrome and my gallbladder are contributing to my symptoms and vomiting. So, all in all, the plan is to start the surgery laparoscopically. Then, Dr. Yang will see if a laproscopic lysis of the ligament of treitz is possible. That is where he can possibly reposition my duodenum and the ligament of treitz to get my duodenum out of the narrowed angle of the aorta and superior mesenteric artery. If that is not possible, and the surgeon will only know once he begins operating, then he will continue with a duodenojejunostomy. A duodenojejunostomy is essentially a bypass surgery where my duodenum will be cut, moved out from between the aorta and SMA, and reattached. Again, hopefully this is all laparoscopic unless Dr. Yang feels he needs to make a larger incision. After correcting the SMA syndrome, he will continue with the cholecystectomy to remove my gallbladder. I know this is definitely a lot of information, but I want to document this step of my journey and reach out to others. Hopefully I can help spread more awareness and knowledge of SMA syndrome to both doctors and people struggling to diagnose or cure their abdominal related issues! |
Author17-year-old small-town girl living life day by day. Archives
January 2017
Categories |








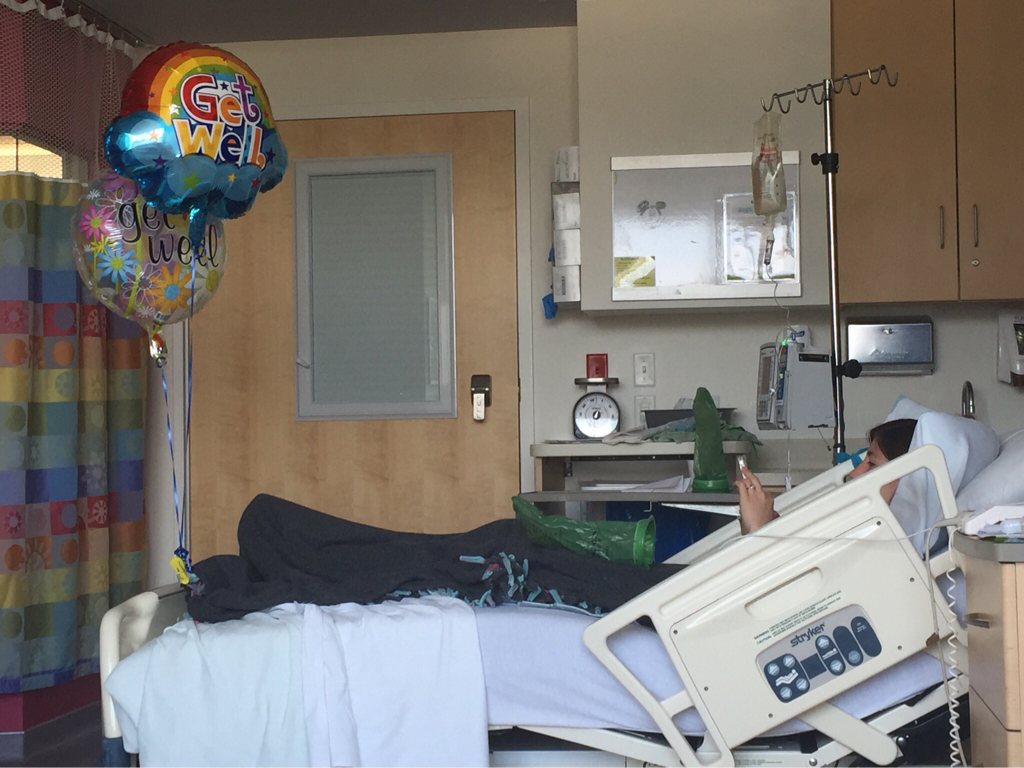








































 RSS Feed
RSS Feed
